- Deep Dive into Pelvic Floor Anatomy: More Than Just a Hammock
- The Mind-Muscle Disconnect: Why Somatic Awareness is Challenging
- 7 Step-by-Step Methods to Identify Pelvic Floor Activation
- 1. The "Stop the Flow" Test (Diagnostic, Not Prescriptive)
- 2. The Elevator Visualization Technique
- 3. The Blueberry / Marble Cue
- 4. The Mirror Biofeedback Method
- 5. Tactile Palpation (External and Internal)
- 6. Breath Synchronization Assessment
- 7. Clinical Biofeedback Devices
- Red Flags: How to Know You Are Doing It WRONG
- The Spectrum of Dysfunction: Hypotonic vs. Hypertonic Pelvic Floors
- Bridging the Gap with Advanced Technology: The Emsella Chair
- What is the Emsella Chair?
- The Science of Supramaximal Contractions
- Why Emsella Chair Treatments Outperform Manual Isolation
- Frequently Asked Questions (FAQ)
- Conclusion
How Do I Know If I'm Activating My Pelvic Floor? Complete Guide & Solutions
Establishing a strong connection with your pelvic floor—the "invisible" foundation of your core—is essential for bladder control, sexual health, and overall structural stability. However, because these internal muscles lack visual feedback, many people struggle to know if they are activating them correctly or merely compensating with surrounding muscles. This guide provides a deep dive into pelvic anatomy and offers seven actionable techniques to help you master the mind-muscle connection. We also explore common pitfalls like "bearing down" and examine how advanced technologies, specifically Emsella chair treatments, are revolutionizing recovery by ensuring perfect, effortless muscle engagement every time.
Deep Dive into Pelvic Floor Anatomy: More Than Just a Hammock
To effectively activate a muscle, you must first understand where it is and what it actually does. The pelvic floor is frequently, and somewhat simplistically, described as a "hammock" of muscles. While this analogy is helpful for basic visualization, it severely understates the anatomical complexity and multi-directional functionality of this region.
The pelvic floor is a dense, three-dimensional web of muscles, ligaments, and connective fascia that spans the bottom of the pelvic basin. It stretches from the pubic bone in the front to the tailbone (coccyx) in the back, and side-to-side between the sitting bones (ischial tuberosities). It does not just passively hold weight; it is a dynamic, reactive suspension system.
Functionally and clinically, the pelvic floor is divided into three distinct compartments, each with specific roles:
1. The Anterior Compartment This section supports the bladder and the urethra. The muscles here are responsible for urinary continence. When these muscles are strong and properly innervated, they maintain a tight seal around the urethra, preventing the involuntary leakage of urine when intra-abdominal pressure suddenly increases—such as when you sneeze, cough, laugh, or jump.
2. The Middle Compartment In females, this compartment supports the uterus, the cervix, and the vagina. In males, it relates to the prostate gland. The muscles in this central zone are crucial for sexual function, reproductive health, and preventing pelvic organ prolapse (a condition where the pelvic organs drop from their normal position and press against the vaginal or rectal walls).
3. The Posterior Compartment This final section supports the rectum and the anal sphincter. The muscles here control bowel movements and the release of flatulence. They must act in a highly coordinated manner, remaining contracted to maintain continence throughout the day, but relaxing entirely to allow for comfortable, strain-free bowel movements.
The primary muscle group encompassing these compartments is the levator ani, which itself is composed of three distinct muscles: the puborectalis, the pubococcygeus, and the iliococcygeus. Together, these muscles must perform a delicate balancing act. They must be strong enough to resist the downward force of gravity and intra-abdominal pressure, yet flexible enough to stretch during childbirth or relax during elimination. When you are trying to "activate" your pelvic floor, you are attempting to consciously command this complex, deep-seated network to perform a synchronized upward and inward lift.
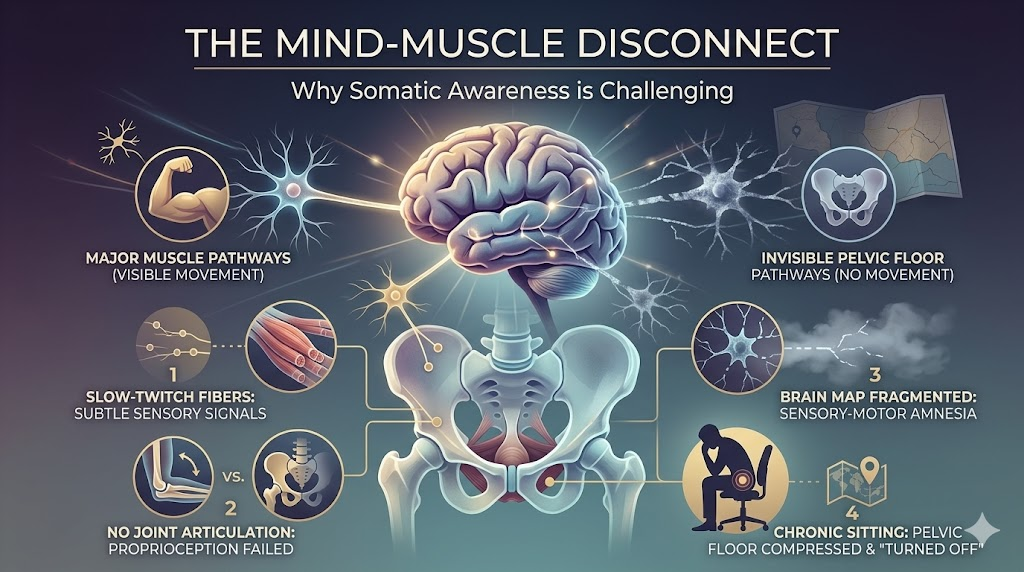
The Mind-Muscle Disconnect: Why Somatic Awareness is Challenging
If the pelvic floor is so vital, why is it so incredibly difficult to feel? The answer lies in the specific type of nerve endings and muscle fibers present in this region, as well as our modern, sedentary lifestyles.
First, the pelvic floor is primarily composed of smooth muscle and slow-twitch (Type I) skeletal muscle fibers. Slow-twitch fibers are designed for endurance rather than explosive power. They are meant to work quietly in the background all day long, maintaining a baseline level of tension (tone) to keep your organs in place. Because they are not designed for massive, rapid, forceful contractions like your quadriceps or pectorals, the sensory signals they send to the brain are inherently much subtler.
Second, the human brain relies on a concept called proprioception—the body's ability to perceive its own position in space. Proprioception is heavily reliant on visual confirmation and joint movement. When you bend your elbow, the brain registers the change in the joint angle and visually confirms the movement of the arm. The pelvic floor, however, is attached to a rigid bony pelvis. When it contracts, no joints bend, and the movement is entirely internal. Without visual confirmation or joint articulation, the brain struggles to map the area accurately.
Finally, chronic sitting plays a massive role in this sensory disconnect. Modern lifestyles force us into chairs for eight to twelve hours a day. When we sit continuously, we compress the pelvic floor and essentially "turn off" the core muscles. Over years and decades, this leads to a phenomenon known as sensory-motor amnesia. The brain simply forgets how to clearly communicate with these nerves, resulting in a numb, disconnected feeling when you finally try to engage them.
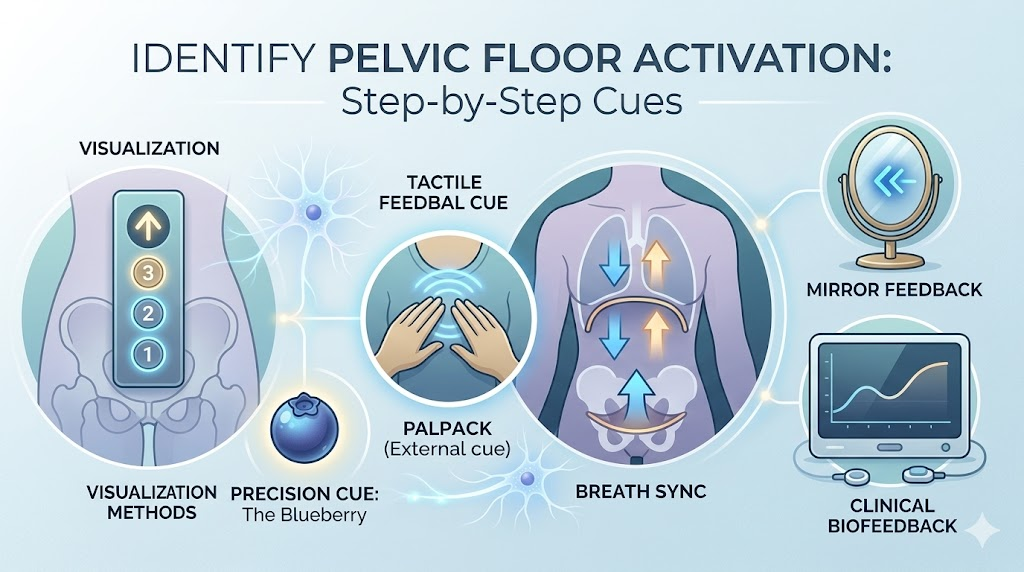
7 Step-by-Step Methods to Identify Pelvic Floor Activation
Regaining control of your pelvic floor requires patience and practice. Because the area is difficult to feel, practitioners have developed a variety of physical cues, visualizations, and feedback mechanisms to help individuals identify the correct sensation. Here are seven detailed, highly effective methods to help you determine if you are activating your pelvic floor correctly.
1. The "Stop the Flow" Test (Diagnostic, Not Prescriptive)
This is perhaps the oldest and most universally understood method for identifying the pelvic floor. While sitting on the toilet, attempt to stop the stream of urine mid-flow.
-
The Sensation: If you successfully stop or significantly slow the flow, you have successfully engaged the anterior compartment of your pelvic floor muscles.
-
Crucial Warning: This is purely a diagnostic test to help your brain locate the muscle. Do not use this as your regular exercise routine. Repeatedly stopping the flow of urine can confuse your bladder's neurological reflexes, leading to incomplete emptying, which increases the risk of urinary tract infections and bladder dysfunction. Use this test once or twice just to find the muscle, then replicate that exact sensation when you are not using the bathroom.
2. The Elevator Visualization Technique
Visualization is a powerful tool for bridging the gap between the brain and internal muscles. Because the pelvic floor needs to lift upward, the elevator analogy is highly effective.
-
The Setup: Sit comfortably upright in a chair with your feet flat on the floor, or lie on your back with your knees bent.
-
The Action: Imagine your pelvic floor is the ground floor of an elevator shaft. Take a deep, relaxed breath in. As you exhale, imagine the elevator doors closing (this represents the tightening of the sphincters). Then, imagine the elevator lifting up to the first floor, then the second floor, then the third floor, deep into your abdomen.
-
The Sensation: You should feel a distinct "drawing in" and "lifting up" sensation deep within your pelvis. There should be no downward pressure. When you inhale again, slowly let the elevator descend back to the ground floor, fully relaxing the muscles.
3. The Blueberry / Marble Cue
This visualization is particularly helpful for isolating the precise muscles without engaging the surrounding areas.
-
The Setup: Lie on your back in a neutral, relaxed position.
-
The Action: Imagine a small blueberry or a glass marble resting just at the entrance of your vagina or rectum. As you exhale, imagine trying to gently pick up that blueberry with your pelvic muscles and draw it upward into your body.
-
The Sensation: Because a blueberry is small and delicate, this cue prevents you from using massive, forceful strength. It encourages a precise, focused, and gentle inward lift. If you squeeze too hard, you would "crush" the blueberry. This helps refine the specific mind-muscle connection.
4. The Mirror Biofeedback Method
Since the brain craves visual feedback, providing it artificially can rapidly accelerate your learning curve.
-
The Setup: In a private, comfortable space, undress from the waist down. Lie on your back with your knees bent and gently spread apart. Use a hand mirror angled so you can clearly see your perineum (the area between the vagina/scrotum and the anus).
-
The Action: Perform the elevator or blueberry cue.
-
The Visual Sensation: If you are doing it correctly, you will actually see the perineum visibly retract and lift inward, moving away from the mirror. The anus should visually pucker and draw tight. If you see the area bulging outward, pushing closer to the mirror, you are performing a Valsalva maneuver (bearing down) and are doing the exercise incorrectly.
5. Tactile Palpation (External and Internal)
Using your sense of touch can provide the physical resistance your brain needs to register the contraction.
-
External Palpation: Place your fingers lightly on your perineum (the central point between the genitals and the anus) over your clothing. When you attempt a pelvic lift, you should feel the tissue draw away from your fingertips.
-
Internal Palpation (For Females): After thoroughly washing your hands, insert one clean, lubricated finger shallowly into the vagina. Attempt to contract the pelvic floor. You should feel the vaginal walls gently squeeze around your finger and a distinct upward pulling sensation toward your head.
6. Breath Synchronization Assessment
The pelvic floor does not work in isolation; it is intimately connected to your diaphragm (the primary breathing muscle). They act like a piston system.
-
The Sensation: Place one hand on your ribcage and one on your lower abdomen. When you inhale deeply, your diaphragm pushes down, which means your pelvic floor must relax and gently expand downward to accommodate the pressure. When you exhale, the diaphragm moves back up, and the pelvic floor should naturally recoil and lift upward. If you are holding your breath while trying to contract your pelvic floor, you are fighting your own anatomy. Correct activation always occurs on the exhale.
7. Clinical Biofeedback Devices
If manual methods fail, clinical intervention can provide definitive answers. Pelvic floor physical therapists utilize sophisticated biofeedback machines. These involve placing small external sensors, or a mild internal probe, that measure the electrical activity of the muscles. The machine translates your internal muscle tension into a visual graph on a computer screen. When you squeeze correctly, the line on the screen goes up. This real-time, objective data is highly effective for retraining the neuromuscular connection.
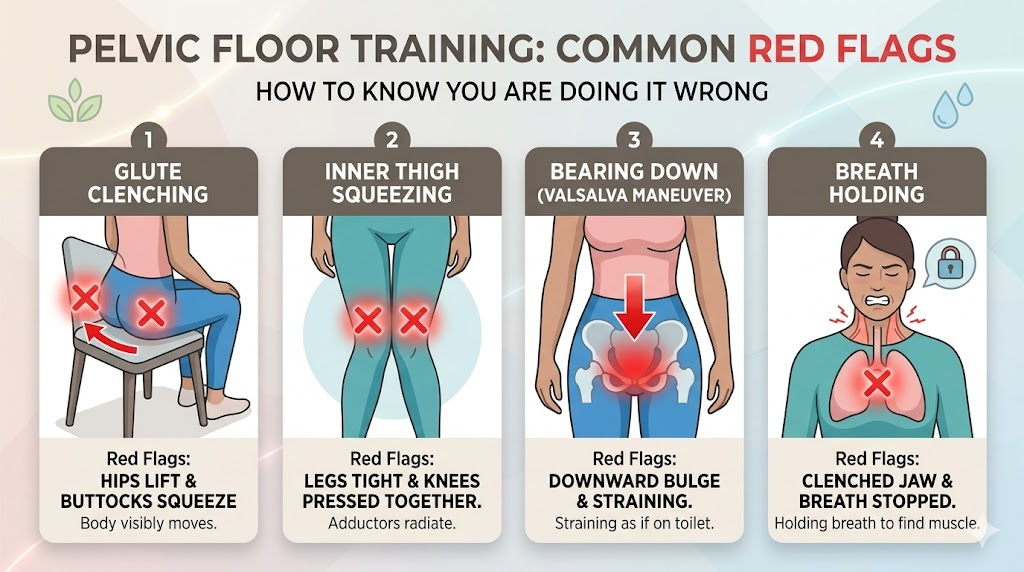
Red Flags: How to Know You Are Doing It WRONG
Just as important as knowing when you are activating the right muscles is knowing when you are compensating with the wrong ones. Because the pelvic floor is weak in many people, the body will naturally recruit stronger surrounding muscles to "cheat" and get the job done. If you experience any of the following, pause, reset, and try again.
-
Co-contraction of the Glutes: Your buttocks are massive, powerful muscles. If you feel your cheeks squeezing together tightly, or if your entire pelvis lifts slightly off the chair when you try to do a Kegel, you are using your glutes, not your pelvic floor. The pelvic floor contraction should be entirely internal; your body should not visibly move.
-
Squeezing the Adductors (Inner Thighs): Similar to the glutes, the inner thighs often try to take over. If you feel tension radiating down the inside of your legs, or if your knees are forcefully pressing together, you are compensating. Try practicing with your legs slightly wider apart to disengage the adductors.
-
The Valsalva Maneuver (Bearing Down): This is the most dangerous mistake. If you feel a downward bulging sensation—similar to the feeling of straining during a difficult bowel movement or pushing during childbirth—you are increasing intra-abdominal pressure without lifting the pelvic floor. Over time, this repetitive downward straining can actually cause or worsen pelvic organ prolapse and stress urinary incontinence.
-
Breath Holding: If you have to hold your breath, clench your jaw, or tighten your neck muscles to feel a contraction in your pelvis, you are not isolating the core correctly. Pelvic floor activation should be a smooth, continuous movement paired with an effortless exhalation.
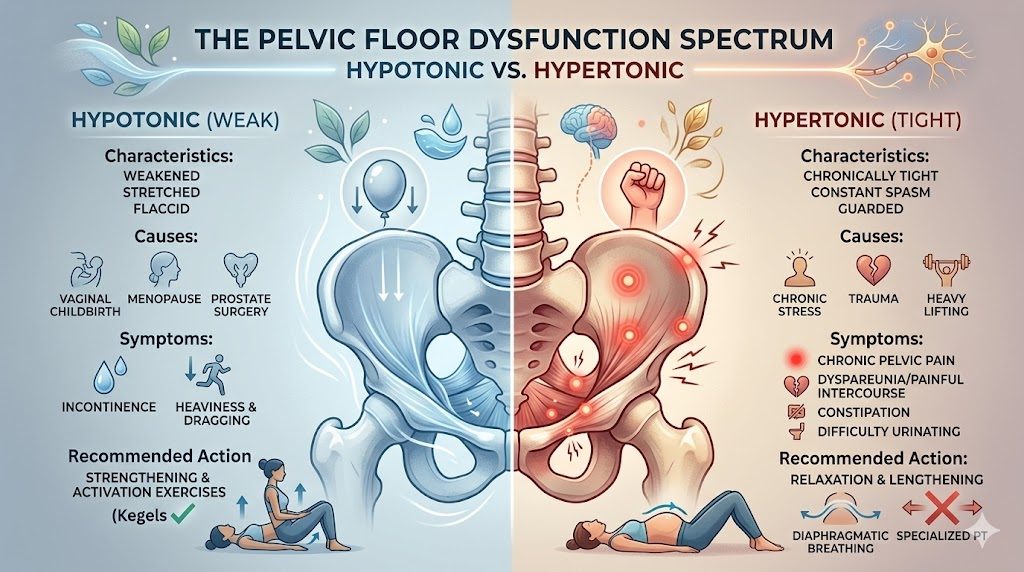
The Spectrum of Dysfunction: Hypotonic vs. Hypertonic Pelvic Floors
It is a common misconception that all pelvic floor issues stem from weakness (a hypotonic state). Consequently, many people blindly perform thousands of Kegel exercises, assuming tighter is always better. In reality, pelvic floor dysfunction exists on a spectrum.
Hypotonic (Weak) Pelvic Floor: This is the classic presentation of a weakened, stretched muscle group. It is incredibly common after vaginal childbirth, during menopause due to estrogen depletion, or following prostate surgery in men. Symptoms primarily include stress urinary incontinence (leaking when coughing or jumping), urge incontinence (a sudden, uncontrollable need to urinate), and a feeling of heaviness or dragging in the pelvic region, indicative of early-stage prolapse. For these individuals, strengthening and activation exercises are the gold standard of conservative care.
Hypertonic (Overactive/Tight) Pelvic Floor: Conversely, many individuals suffer from a pelvic floor that is chronically tight, locked in a state of continuous spasm, and unable to relax. This is often linked to chronic stress, trauma, heavy weightlifting without proper core management, or conditions like endometriosis. Symptoms of a hypertonic pelvic floor include chronic pelvic pain, painful intercourse (dyspareunia), severe constipation, and difficulty initiating a stream of urine.
Crucial Insight: If you have a hypertonic pelvic floor, performing traditional activation exercises (Kegels) will actually make your symptoms worse. You do not need to learn how to contract; you need to learn how to consciously relax and lengthen the muscles through deep diaphragmatic breathing and specialized physical therapy. This is why accurately identifying your specific baseline is so vital before beginning any intensive exercise regimen.
Bridging the Gap with Advanced Technology: The Emsella Chair
Despite the best efforts with visualizations, biofeedback, and physical therapy, achieving optimal pelvic floor strength manually can take months of dedicated, daily practice. Even then, human error, muscular fatigue, and the inherent difficulty of the mind-muscle connection can limit the overall effectiveness of manual isolation.
This is where the intersection of wellness and advanced engineering has provided a revolutionary solution. For individuals struggling to identify their pelvic floor, or those looking for an exponentially more powerful rehabilitative tool, the emsella chair represents the pinnacle of non-invasive pelvic health technology.
What is the Emsella Chair?
At first glance, the device simply looks like a modern, sleek chair. However, beneath the seat lies highly sophisticated medical technology. The emsella chair utilizes High-Intensity Focused Electromagnetic (HIFEM) technology to directly stimulate the nerves of the pelvic floor, bypassing the brain entirely.
The Science of Supramaximal Contractions
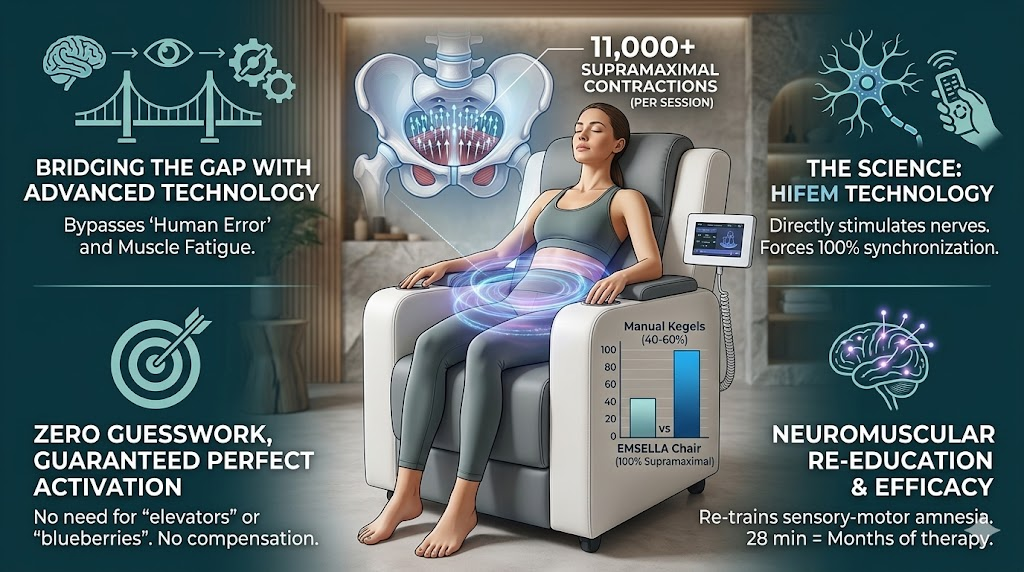
When you perform a manual Kegel exercise perfectly, you are engaging roughly 40% to 60% of the muscle fibers in your pelvic floor. Furthermore, you can only hold that maximal tension for a few seconds before the muscle fatigues.
HIFEM technology works on a vastly different scale. When you sit on the emsella chair—fully clothed and comfortably positioned—the device emits focused electromagnetic waves that penetrate the pelvic basin. These waves force the entire network of pelvic floor muscles to contract simultaneously and at 100% capacity. These are known as supramaximal contractions, a level of muscular tension that is physiologically impossible to achieve through voluntary neurological control.
During a standard 28-minute session, the emsella chair induces the equivalent of over 11,000 perfect, supramaximal Kegel exercises. The electromagnetic field continuously contracts and releases the muscles, building dense myofibril structures, improving localized blood flow, and rapidly re-educating the neuromuscular pathways.
Why Emsella Chair Treatments Outperform Manual Isolation
-
Zero Guesswork: Because the machine directly stimulates the motor neurons, you do not need to worry about the "elevator" or the "blueberry." The device forces the correct muscles to activate perfectly every single time, completely eliminating the risk of co-contracting the glutes or bearing down.
-
Neuromuscular Re-education: For those who suffer from sensory-motor amnesia, emsella chair treatments force the brain to recognize the pelvic floor again. After a few sessions, patients frequently report that they can finally "feel" their pelvic floor and can perform manual Kegels much more effectively because the neurological pathways have been "woken up" by the intense stimulation.
-
Time Efficiency and Efficacy: Achieving the muscle hypertrophy and tone generated by 11,000 supramaximal contractions would take months of rigorous, error-free manual therapy. The technology condenses months of physical therapy into brief, painless, half-hour sessions, making it highly appealing for busy individuals and a highly effective clinical intervention for stress and urge incontinence.
For modern wellness centers and clinical practices, the shift toward technologies like the emsella chair represents a fundamental upgrade in how we treat the invisible core, offering tangible, rapid results where manual therapies often stall.
Frequently Asked Questions (FAQ)
1. How long does it usually take to feel results from manual pelvic floor exercises?
If you are performing manual exercises correctly and consistently (3-4 times a day), you may begin to notice minor improvements in bladder control and core stability within 4 to 6 weeks. However, significant structural and muscular hypertrophy usually requires 3 to 6 months of dedicated practice.
2. Are emsella chair treatments painful?
No, the treatment is entirely non-invasive and generally completely painless. Patients remain fully clothed. You will feel intense muscular contractions and a localized tingling sensation, but it should not cause pain. Most individuals read a book or relax during the 28-minute session.
3. Can I do pelvic floor exercises while pregnant?
Yes, in fact, it is highly recommended. Strengthening the pelvic floor during pregnancy can help carry the increased weight of the baby, reduce the risk of third-trimester incontinence, and aid in postpartum recovery. However, you should always consult your OB-GYN before starting any new routine during pregnancy.
4. How do I know if I need manual therapy versus technological intervention?
If you can easily identify your pelvic floor using the tactile or visualization methods mentioned above, and your symptoms are very mild, manual exercises may be sufficient. However, if you struggle to feel the contraction, suffer from significant incontinence that impacts your daily life, or are looking for rapid, guaranteed muscle engagement, advanced technological interventions are generally the recommended path.
5. Is it normal to feel sore after activating the pelvic floor? J
ust like any other muscle in your body, the pelvic floor can experience Delayed Onset Muscle Soreness (DOMS) if it is overworked. Mild aching or a feeling of heaviness after a rigorous session of Kegels or an initial technological treatment is normal. However, sharp pain or cramping indicates that you need to rest and allow the tissue to recover.
Conclusion
Understanding and isolating your pelvic floor is a vital component of long-term structural health, core stability, and personal confidence. By utilizing visualization techniques, tactile feedback, and proper breath synchronization, you can begin to rebuild the neuromuscular pathways to this essential, yet invisible, muscle group.
Ready to elevate your wellness center or clinical practice with state-of-the-art non-invasive technology? With over a decade of dedicated experience in manufacturing top-tier beauty and wellness equipment, we provide direct-from-source solutions that prioritize technical excellence and reliable results. Contact us today to learn more about integrating advanced technologies like the emsella chair into your facility, and discover how our factory-direct technical upgrades can enhance your service offerings, improve patient outcomes, and build lasting client trust.




Air Pressotherapy Machine
Who can benefit from using this air pressure body massage machine?
Ideal for beauty salons, spas, physiotherapy centers, and wellness clinics aiming to provide detox, relaxation, or slimming treatments.
ulthra超声刀
How long do results last?
Results can last 12–18 months, depending on individual skin conditions and lifestyle factors.
JHF-51
What is the benefit of privacy detection technology?
Privacy detection improves treatment safety and discretion, especially for intimate and sensitive procedures.
L50
Is the Cellulite Removal Tightening Therapy painful?
No, the treatment is non-invasive and comfortable, with adjustable intensity for different clients.
VM-1
Who is this cryolipolysis machine suitable for?
It is suitable for clinics, slimming centers, beauty salons, and professional aesthetic practitioners.




Get more information
If you have any comments or good suggestions, please leave us a message; later our professional staff will contact you as soon as possible.
© 2025 HUIMAIN. All Rights Reserved. Privacy Policy | Terms and Conditions | Sitemap




Facebook
Instagram
Medical beauty equipment factory
huimain Medical beauty equipment factory
beauty machine supplier
Whatsapp: +8619124004543